Paola Ash
Chiropodist Fungal Nail Treatment
“Why are my nails yellow?” “Why do I have white spots on my nails?”
Fungal nail infections are common. Although they can also happen to fingernails they tend to be more prevalent in the toenails. This could be partly due to feet being covered during the day, and circulation of blood to the toes may be diminished in certain situations to make the surroundings more favorable for fungi called dermatophytes to grow. Fungi thrive in warm, dark and humid conditions that can cause infections to the nails. Fungal nails are more prevalent with advancing age. Males are more susceptible than women.
Toenail fungus can be deceiving at first. Initially, you might believe that you have maybe noticed a tiny change in the colour of the affected nail. However, this may be overlooked for months since the fungal infection may begin in only one part of the nail. In time, further changes in the appearance of your nails appear.
Furthermore, color changes as well as thickening or broken nails are characteristic. As the disease progresses, the nails may begin to soften get more distorted arising from the nail plate beneath. Also, debris accumulates and, in many cases, the odour of nail fungus can be prominent. Sometimes, it may also be the cause of athlete’s foot or vice a versa. Fungal nails are very difficult to treat, oftentimes returning is not undertaking thorougly.
At this point, some believe that cutting or filing the nail sufficiently, the fungus will go away. This is not the case.
Signs and Symptoms of fungal nail infections
Is your toenail soft ? Fungal nail infections can cause a range of changes in the affected toenail, which include:
- brittle, crumbling nail edges;
- yellow or white spots or streaks under the tip of the nail;
- nail thickening and roughness;
- nail discoloration (nails may turn yellow, white or brown);
- tenderness and pain; and
- separation of the nail from the nail bed.
Clinical features of onychomycosis
Fungal nails may involve a single nail or multiple nails. It may also affect the skin that surrounds it.
Clinical types include:
- Superficial white onychomycosis — flaky, white patches and pits are visible on the top of the nail plate.
- Lateral and distal subungual onychomycosis — the distal end and sides of the nail lift or become discoloured and crumble.
- Superficial white onychomycosis — flaky, white patches and pits appear on the top of the nail plate.
- Proximal subungual onychomycosis — the proximal nail plate near the lunula becomes thickened and discoloured. This pattern of disease can relate to underlying HIV infection.
- Endonyx onychomycosis — milky white discolouration of the nail plate develops without subungual hyperkeratosis or onycholysis.
- Onychauxis.
Risk factors of fungal nails
Here are some factors that would place you at higher risk of developing a fungal nail infection:
- if you have diabetes;
- if you have problems with your circulation;
- having frequently moist skin, often due to excessive sweating;
- being older than 60;
- if you have a problem with your immune system;
- always wearing footwear that is closed-in, doesn’t absorb sweat, and has poor ventilation; and
- working in a moist or humid environment.
People who are active in sports such as running may be at bigger risk of getting a fungal toenail infection since they often damage their toenails, which would make an opening for infections to get under the toenail. Also, wearing running shoes regularly means that the feet are often exposed to moist, warm conditions, ideally where fungal infection grows.
Moreover, people who commonly have wet hands, such as professional cleaners and cooks, are at increased risk of having a fungal infection in the fingernails.
Chiropodist Fungal Nail Treatment London
What is the best way to treat fungal nail infection? Here are best fungal nail treatments:
Topical Antifungal Treatments
A topical treatment may be applied if the infection is superficial or affects only the end of the nail (less than half the total nail area). Nevertheless, there are times that these treatments are not enough to penetrate the nail sufficiently to treat the fungal infection.
There are also some antifungal nail lacquers that are available for use to treat fungal nail infections. Treatment with these topical nail lacquers should be continuous until a healthy nail re-grows (2 to 12 months). Avoid using false nails, nail polish, or other cosmetic products on treated nails. Also, women who are pregnant or breast feeding, and children are prohibited in using these treatments.
There is also another topical treatment that is available as a Fungal Nail Treatment Set. The set consist of 2 treatment phases: first is softening and removing the infected parts of the nail with urea ointment and a plastic nail scraper (2-3 weeks); then applying an antifungal cream to the nail bed to treat the fungal infection (4 weeks). Also, this treatment may not be suitable for pregnant or breast feeding women or children.
The possible side effects from local (surface) treatments include skin infection, skin rashes, and irritation around the nail as well as nail discoloration.
Pros of Topical Anti- Fungal Therapy with Burring of the Nail
- Allows adequate penetration of topical fungal medication
- Reduce nail thickness
- Assessment is required prior to application
- Cost effective
Topical treatments
There is a treatment for Fungal Nail Infection that is obtainable at pharmacies. This treatment is applied twice a day for a minimum of 3 months to the affected nail(s), using a special applicator. It can help treat fungal nail infections by penetrating the nail, making it more acidic and hostile to fungal growth.
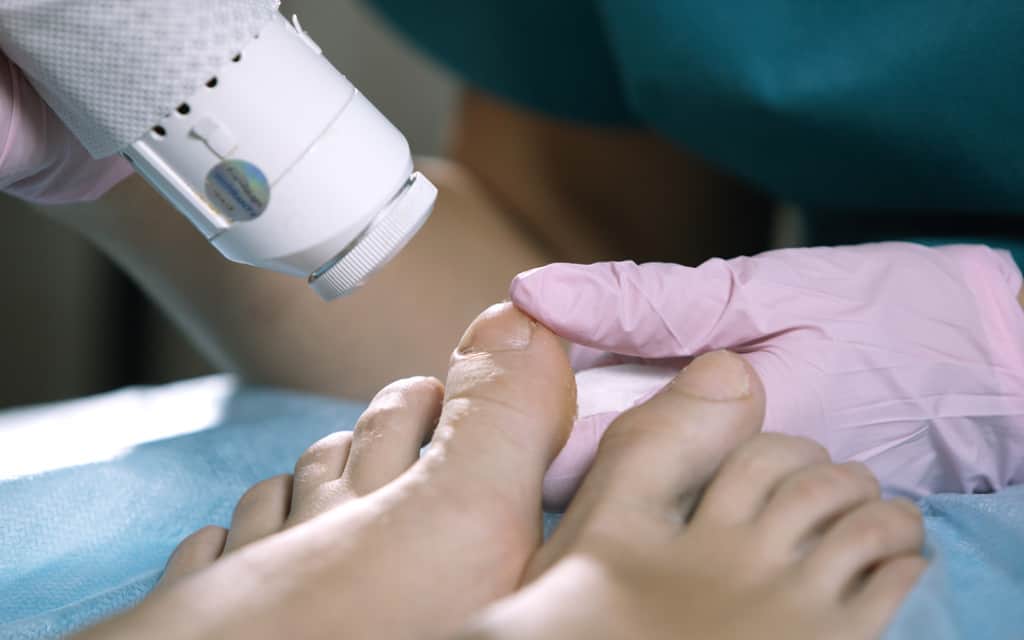
Laser treatment
Laser therapy is a modern treatment for fungal nail infections. The podiatrist may require to have the treatment once every 3 months for up to 12 months. Toenail fungus laser treatment works by heating up the nail layers exactly to the fungus and trying to destroy the genetic material responsible for fungus development and survival.
At The Chelsea Clinic, our podiatrists with years of experience in podiatry service are experts already in fungal nail treatment. They have treated many patients with this kind of condition. Some opted to do fungal nail laser treatment. Laser fungal nail treatment needs no recovery period.
Oral Antifungal Medicines
More severe infections (involves the base of the nail or the nail-bed) normally need oral antifungal medicine. Some factors need to be considered before the nail doctor will give prescription. The exact choice will depend whether you have other medical conditions, on which fungus is causing the problem, if you are pregnant or planning to become pregnant (some treatments may affect the unborn baby), and what other medicines you are currently taking. The treatment lasts from 6 weeks to 12 months or more. It depends on the fungus in question and the place of the infection, with fingernails usually responding faster than toenails. It is also to be noted that oral antifungal medicines are associated with a number of potential side effects. This includes skin rashes, headaches, liver damage, gastrointestinal upsets (such as diarrhea) and heart problems.
Nail Removal
When medical treatments have been tried and don’t work, the last resort is to remove the nail. It is either surgically removed with or without chemicals. A new nail should grow back in place if it has not had chemical treatment. There is a 50% chance the nail will grow back not infected.
Your nail specialist doctor can recommend the best fungal nail treatment for severe cases.
How to prevent fungal nail infections?
Here are some tips on how to prevent fungal nails and its recurrence:
- Keep your feet dry and cool.
- Avoid using occlusive footwear and excessive sweating
- Avoid having nail trauma by trimming nails short
- Use prophylactic antifungals in feet and in between the toes
- Avoid unhygienic cosmetic nail practices
- Using non-slip sliders/flip-flops in swimming pools and public gyms
- Discard or treat infected footwear and socks
- Addressing poorly controlled diabetes.
- Patient counselling for optimal onychomycosis therapy to improve observance.
When you think about this, it is crucial to assess your footwear and to ensure that the shoes you are wearing are not too old (a dermatophytes hive). Also, with one set of shoes, if we mix the pair with another every second weekday to ensure that we can encourage a 24- day period that allows the shoes to breathe making your shoes more healthy less bacterially and fungally loaded.
Regularly changing your footwear, or cleaning suede or leather shoes once in a while will help improve the cleanliness of footwear. Socks that are washed at high temperatures and changing socks frequently is also advised. Make sure that all visits to the pool are carried out with flip flops on or from the change rooms, and as well into and out of showers. Also, keeping your feet clean and dry is best for fungal nails. An effective anti fungal spray for nails is proven to provide care for unsightly toenails prone to fungal nail infections.
Diagnosis of Fungal Nails
A number of nail disorders may look like fungal nail infections such as psoriasis. Hence, it’s important to have a precise diagnosis from your nail doctor so you don’t waste time and money on treating the wrong condition. Also, nail fungus is much better to be diagnosed and treated in the early stages. Our qualified podiatrists can diagnose a fungal infection from a physical examination, and if needed, we can have a sample of the nail tested by a lab to confidently confirm the diagnosis.
Diagnosis of Onychomycosis
It can involve physical examination of all nails, and a number of tools, like those enumerated below.
Dermoscopy
Dermoscopy may be able to differentiate between traumatic onycholysis, onychomycosis, and melanonychia. Common dermatoscopic findings include discolouration, subungual keratosis, linear bands which round proximally and taper distally, non-longitudinal homogenous or reverse triangular patterns, nail plate scales, and white/yellow streaks.
The pattern of fungal invasion is further divided into:
- Superficial onychomycosis – white patches that affects the distal nail
- Endonyx onychomycosis – infection of the nail plate but not the nail bed
- Proximal subungual onychomycosis – involvement of the proximal nail fold under surface to distal
- Mixed pattern onychomycosis.
Mycology specimens
Clippings should be taken from the crumbling free edge of the affected nail. - The most proximal areas of the dystrophic nail give the best yield on microscopy and culture; they can accessibly be obtained by scraping as proximally as possible under the nail with the hooked end of a clean nail file.
- Microscopic examination reviewed under light microscopy using potassium hydroxide (to dissolve keratinocyte material) is a quick test to assess for the presence of fungal hyphae, although it lacks specificity and sensitivity.
Fungal culture testing
Fungal cultures can recognize the causative organism and is the standard diagnostic test. However, results can take weeks and a large specimen collection may be necessary.
Samples should be taken prior to starting any treatment.
Polymerase chain reaction testing (PCR)
PCR testing quickly finds the offending organism and is highly specific and sensitive. It is becoming more commonly available, however is more expensive than microscopy or fungal culture testing.
Outlook
Patients with diabetes are more susceptible to nail complications and should consult to a podiatrist. Nonetheless, fungal nail infections generally have a good prognosis if treated promptly.
The treatment can take a longer time to fully cure the fungal infection, and may need further rounds of treatment. Moreover, complications in some severe cases may include nail damage or may be permanent loss, or spread of the infection. There is also a small chance that it can develop to cellulitis. Hence, it is really important to see a nail doctor, foot specialist, chiropodist or podiatrist to correctly assess your fungal nails.
We can discuss and go through a number of treatment options for you and tailor whichever treatment is best suited to your individual needs. – South Kensington Podiatrist
Chiropodist fungal nail treatment
Check our blog about Fungal Nail Infection here https://www.thechelseaclinic.uk/fungal-nail-infections/
Read our blog about Ingrown Toenail here https://www.thechelseaclinic.uk/ingrown-toenails/
Check our article about our Nail Surgery here https://www.thechelseaclinic.uk/nail-surgery/
Learn more about Plantar Fasciitis here https://www.plantarfasciitisorthotics.co.uk/treatments/plantar-fasciitis
Contact Us
Now offering home visits and online consultations
Tel: +44 (0) 207 101 4000 WhatsApp: +44 (0) 778 066 5223 Email: info@thechelseaclinic.uk
From the Blog

The Microvasculature of the fingertips and toetips
The Microvasculature of the fingertips and toetips The microvasculature of the fingertips and toetips plays a crucial role in maintaining the health and function

Syphilitic paronychia
Syphilitic paronychia Syphilitic paronychia, though rare, is a manifestation of syphilis, a sexually transmitted infection caused by the bacterium Treponema pallidum. Syphilis can have

Its Wimbledon and Tennis Leg Injury
Its Wimbledon and Tennis Leg Injury Wimbledon Tennis starts tomorrow. As such we are talking about none other…than Tennis Leg! You are just about to
